Health Savings Account FAQs
At HSA Bank, we’re working toward a world where everyone is confidently engaged with their health and wealth. By delivering personalized insights, experiences and solutions, we make it simple for our nearly 4 million members nationwide to drive value and tangible outcomes. As a leader in health accounts for over two decades, we have the depth and breadth of expertise that matters most. We are devoted to delivering an outstanding user experience and our offerings in the healthcare savings space drive down healthcare costs, increase access, and assist with decision-making for individuals, employers and partners. As of December 31, 2025, HSA Bank had $15.7 billion in total footings comprising $9.2 billion in deposit balances and $6.5 billion in assets under administration through linked investment accounts and is a division of Webster Bank, N.A., Member FDIC Plan Administrative Services and Benefit Services are administered by Webster Servicing LLC.
The main requirement for opening an HSA is having an HSA-eligible health plan, typically a high-deductible health plan (HDHP), Bronze plan or Catastrophic plan, that meets IRS guidelines for the annual deductible and out-of-pocket maximum. To be an eligible individual and qualify for an HSA, you must also meet the following requirements.
- You must have a valid email address, Social Security Number and a primary residence in the United States.
- You must be covered by the HSA-eligible health plan on the first day of the month in which you plan to start contributing to your HSA.
- You can’t be covered by any other type of health plan, including Medicare Part A or Medicare Part B.
- You can’t be covered by TRICARE.
- You can’t have used your medical benefits from Veterans Administration for any non-service-connected disabilities at any time during the previous three months (to contribute to an HSA). Note: Title 38 of the United States Code, Section 101(17) defines "non-service-connected" as, with respect to disability, that such disability was not incurred or aggravated in line of duty in the active military, naval, or air service.
- You can’t be claimed as a dependent on another person's tax return.
- You aren’t covered by a general purpose healthcare Flexible Spending Account (FSA) or Health Reimbursement Account (HRA). Alternative plan designs, such as a limited-purpose FSA or HRA, might be permitted.
HSA Bank’s routing number is 075907947.
HDHPs, as well as Bronze and Catastrophic plans, are HSA-eligible health plans that satisfy certain requirements for deductibles and out-of-pocket expenses. They typically feature higher deductibles and lower premiums than traditional insurance plans and are the only plan type that can be combined with an HSA. View the IRS guidelines and eligible expenses.
In addition to your HSA-eligible health plan, you may have coverage from "permitted insurance," which is coverage related to compensation from workers' compensation, tort liabilities, liabilities relating to ownership or use of property, insurance for a specified disease or illness and insurance that pays a fixed amount per day of hospitalization. Coverage for accidents, disability, dental care, vision care, Direct Primary Care (DPC) arrangements, telehealth services or long-term care does not disqualify you from opening an HSA.
No. Each spouse must open a separate HSA. You can, however, give your spouse access to your HSA by designating them as an authorized signer on the account.
Anyone may contribute to your HSA on your behalf, as long as you are HSA-eligible and the amount is within the annual IRS contribution limits.
No, as long as you are eligible to contribute. Contributions may be made by you, or on your behalf, even if you are retired, have no income or your income is less than your contributions.
Yes. The IRS determines the maximum amount that can be contributed to an HSA during the calendar year. View the contribution limits.
Eligible individuals over the age of 55 (or turning 55 during the year) are allowed to make additional "catch-up" contributions to their HSAs. The catch-up amount is $1,000. Eligible spouses over 55 can only make catch-up contributions to their account. Catch-up contributions must be prorated as well. If you do not maintain HSA-eligible coverage through the end of the following year, the contributions exceeding the prorated amount for the months of actual eligibility become taxable income and are subject to penalty.
If you drop your HSA-eligible health plan during the year, you must prorate your HSA contributions to avoid tax penalties. The below examples show a calendar year taxpayer whose coverage terminated on the last day in September.
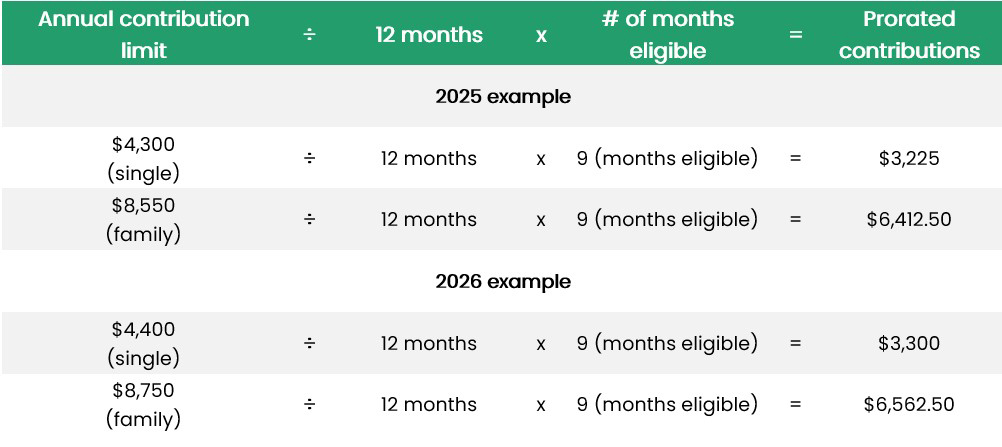
Mid-year Coverage
You can contribute the maximum amount for the year if you’re covered by the first day of the last month of your tax year (December 1), and provided you maintain HSA-eligible coverage until December 31 of the following year. This rule can also be applied to $1,000 catch-up contributions for accountholders aged 55 and older.
Health Plan Status Change
If you begin the year with family coverage and switch to single coverage in July of that year (for example), you are eligible to contribute half of the family coverage maximum and half of the individual coverage contribution maximum.
If you begin the year with single coverage and switch to family coverage by December 1 of that year, you are eligible to contribute the maximum family amount for that year provided you maintain HSA-eligible coverage until December 31 of the following year. This is covered under the “Full contribution” rule and can also be applied to $1,000 catch-up contributions for accountholders aged 55 and older.
Note: HSA Bank does not provide legal or tax advice. Please contact your tax professional with any tax-related questions.
Yes, yearly contributions should be made by your tax filing deadline, generally April 15 of the following year.
If your HSA contributions exceed the IRS contribution limits, you must report the excess amount as gross income on your income tax. You will also have to pay additional excise tax on this amount. However, you can remove the excess contributions by submitting an Excess Contribution Removal Form to us within that tax year.
You can pay for a wide range of IRS-qualified medical expenses with your HSA, including many that aren't typically covered by health insurance plans. This includes deductibles, co-insurance, prescriptions, dental and vision care and more. For a complete list of IRS-qualified medical expenses, visit irs.gov or visit our qualified medical expense page.
Generally, health insurance premiums ARE NOT considered IRS-qualified medical expenses, UNLESS they are for:
- Qualified long-term care insurance
- COBRA health care continuation coverage
- Health care coverage while an individual is receiving unemployment compensation
- Direct Primary Care (DPC) arrangements
For individuals over 65, the following premiums ARE considered IRS-qualified medical expenses:
- Medicare Parts A, B, D, Medicare HMA
- Employee portion paid for employer-sponsored health insurance
- Employee portion paid for employer-sponsored retiree health insurance
Yes, as long as the IRS-qualified medical expenses were incurred after your HSA was established, you can pay them or reimburse yourself with HSA funds at any time. Just be sure to keep sufficient records to show that these expenses were not previously paid for by another source or taken as an itemized deduction in any prior tax year.
As the HSA accountholder, you are responsible. So, it's important to keep records of the IRS-qualified medical expenses you pay for with your HSA in order to exclude those dollars from your gross income.
HSA funds that are used to pay for non-IRS-qualified medical expenses are considered part of your gross income and subject to tax.* Exceptions include HSA distributions that are made after an accountholder's death, disability or after they turn 65.
*HSA contributions and earnings aren’t subject to federal taxes and aren’t subject to state taxes in most states. Contact a tax professional for information about your state.
Yes. You’re able to transfer or rollover funds from an MSA or HSA with another custodian to your current HSA at HSA Bank. You can transfer funds at any time, but you’re limited to one rollover per 12-month period, and the rollover must be completed within 60 days. For more information and step-by-step instructions regarding each process, please visit our dedicated transfer/rollover page.
Yes. Money spent on ineligible costs before age 65 is subject to income tax plus a 20% penalty. After you turn 65, you won’t pay the penalty, but the distribution will still be subject to income tax.
You can use HSA funds to pay for Medicare premiums, including Medicare Part B, which covers outpatient care, and Part D, which covers prescription drugs (most people don't pay premiums for Part A). You can't, however, use the funds for premiums for supplemental, or Medigap, policies.
Flexible Spending Account FAQs
-
Employees set aside funds on a pre-tax basis each year into their Flexible Spending Account (FSA) and subsequently access those funds for IRS-qualified healthcare expenses incurred within the Plan Year.
-
Using an FSA is great way for employees to stretch their benefit dollars. Employees use before-tax dollars in their FSA to reimburse themselves for eligible out-of-pocket medical and dependent care expenses. That means they can enjoy tax savings and increased take-home pay by reducing FICA taxes. And that makes real sense.
-
With an FSA, you elect to have your annual contribution deducted from your paycheck each pay period, in equal installments throughout the year, until you reach the yearly maximum that you have specified. The amount of your pay that goes into an FSA will not count as taxable income, so you will have immediate tax savings.
-
FSA dollars can be used during the plan year to pay for qualified expenses and services. And at the end of the year, you can roll over (or carryover) a certain amount to the next plan year, provided your employer's plan allows this. View the maximum IRS carryover amount.
-
Annual participant contributions are limited by the Internal Revenue Service. To view current IRS limits, visit the IRS Guidelines and Eligible Expenses page for more information.
A Healthcare FSA allows reimbursement of qualifying out-of-pocket medical expenses. Common eligible expenses include dental treatment, orthodontia, prescription drugs, diagnostic services, hospital services and surgery, laboratory fees, obstetrical expenses, chiropractic care, physical therapy, eye examinations, glasses, contact lenses, laser eye surgery, hearing aids, smoking cessation programs, and weight loss programs to treat obesity, to name a few.
A Limited Purpose Medical FSA works with a qualified high deductible health plan (HDHP) and Health Savings Account (HSA). A limited purpose FSA only allows reimbursement for vision and dental expenses.
A Dependent Care FSA allows reimbursement of dependent care expenses, such as daycare, incurred by eligible dependents. A Dependent Care FSA provides pre-tax reimbursement of out-of-pocket expenses related to dependent care. This benefit may make sense if an employee (and spouse, if married) is working or in school, and:
-
Their dependent children under age 13 attend daycare, after-school care or summer day camp.
-
They provide care for a person of any age whom they claim as a dependent on their federal income tax return and who is mentally or physically incapable of caring for himself or herself.
With an FSA from HSA Bank, employees can:
-
Pay for IRS-qualified expenses with pre-tax dollars.
-
Enjoy significant tax savings with pre-tax deductible contributions and tax-free distributions.
-
Enjoy secure access to accounts using our convenient Member Website available 24/7/365.
-
Quickly and easily access funds with the HSA Bank Health Benefits Debit Card used at point of sale, or have funds directly deposited to a bank account through online distribution.
-
File claims easily online or via the mobile app, with approval determined based upon eligibility and availability of funds.
-
Store and view healthcare spending data in unique ways, to truly engage in management of the FSA account and be aware of the healthcare expenses they are experiencing over time.
-
Protect the environment by using paperless summaries available online and direct deposit for reimbursements.
A Healthcare FSA could save employees money if they or their dependents:
-
Have out-of-pocket expenses like co-pays, coinsurance, or deductibles for health, prescription, dental or vision plans
-
Have a health condition that requires the purchase of prescription medications on an ongoing basis
-
Wear glasses or contact lenses or are planning LASIK surgery
-
Need orthodontia care, such as braces, or have dental expenses not covered by your insurance
Health Reimbursement Arrangement FAQs
Health Reimbursement Arrangements (HRAs) provide an effective way for your business to reduce its employee healthcare costs without reducing employee benefits. If you’re looking to change or expand your employee healthcare options, HSA Bank has your HRA solution. Benefits for your organization:
-
Save money with lower insurance premiums for employees with high deductible health plans.
-
Free Human Resources staff with a centralized Employer Administration website to help manage your plan.
-
Save administrative time with an HRA solution that accepts plan changes from payroll systems and handles a wide variety of HRA plan designs, including deductible, coinsurance, and copayment design options.
-
Go green with direct deposits and the elimination of manual, paper-based claims processes.
-
Offer an employer contribution amount in annual, monthly or custom accruals.
-
Offer flexible benefit options to meet every situation with the ability to stack an HRA with an FSA.
-
Vary your funding amounts based on your employees’ qualifying tiers.
-
Customize eligible expenses and reimbursement amounts.
Our HRA solution will:
-
Give you a choice of several HRA plan designs, such as HRA with individual/family deductible, HRA with copayments for specific expense types, HRA with percentage payouts, or HRA with embedded deductible.
-
Allow you to manage HRA funding, schedules, and reimbursement rules within the interface and allow for tiered funding (individual, individual + spouse, etc.), custom funding schedules, and individual/member maximums.
-
Accept wellness incentive contributions into an HRA to further employee engagement in their healthcare.
-
Recognize significant tax savings with pre-tax, deductible funding and tax-free distributions used for IRS-qualified plan expenses.
-
Quickly and easily access funds with the HSA Bank Health Benefits Debit Card used at point of sale, or have funds directly deposited to a bank account.
-
Enjoy secure access to accounts using a convenient Member Website available 24/7/365.
-
Easily file claims online or via the mobile app with the system determining approval based on eligibility and availability of funds.
-
Stay up-to-date on balances and any actions required with automated email alerts, convenient member home page messages, and access to account balance information via your mobile devices.
-
Get one-click answers to your benefits questions.
-
Protect the environment by using paperless summaries available online.
Benefits Card FAQs
A stacked payment card is one debit card that can be used to pay for approved healthcare expenses across all your HSA Bank accounts. The card’s technology can auto-substantiate transactions and knows which account to distribute funds from.
Our debit card uses IRS-approved solutions to automatically approve the eligibility of purchases or payment for services; this is called auto-substantiation. The card uses five different automatic technologies that will recognize and compare transactions to separate eligible purchases from non-eligible purchases. Once a transaction has been substantiated, transactions for the same amount in the same setting don’t require another review.
In addition to providing a seamless transaction experience, auto-substantiation is critical because the IRS requires 100% of FSA and HRA transactions be substantiated. A high auto-substantiation rate is the single biggest success factor for any benefit card program. HSA Bank is proud to deliver an 85-95% auto-substantiation ratio, which is among the highest in the industry.
If your transaction is not auto-substantiated, you (or the secondary cardholder) will receive a series of three notifications starting five days after the transaction to manually substantiate. If documentation is not received, the claim is denied, and you’ll be sent a letter asking you to repay the plan. You can upload documentation in your account, whether online or through the app, by email or mail. Every effort is made to avoid debit card suspension; however, debit card use may be temporarily suspended until the transaction has been satisfied with documentation or the plan is repaid.
Convenience and simplicity. HSA Bank’s stacked card provides seamless, auto-substantiated transactions that are automatically charged to the proper account according to priorities set by the plan. It also provides a convenient payment method that removes the need for reimbursement and the hassle of continually filing claims. One card, one payment method and zero hassles.
Transactions made using an HSA Bank stacked card deliver an 85-95% auto-substantiation ratio — among the highest in the industry — which decreases paperwork and increases member satisfaction. Our 24/7 Client Assistance Center phone number and website are included on the back of the card for convenient consumer support.
Yes, you can order a Benefits Card for your spouse or your eligible dependents who are 18 years old or older. Once a dependent is no longer on your health plan, it’s your responsibility to request the Benefits Card be closed.
Yes. You can report your card lost or stolen and/or order a replacement card in your online account under Settings, Debit Cards.
No, new Benefits Cards aren’t automatically sent if you update your address. You’ll need to request a new card through your online account under Settings, Debit Cards.
Setting up a PIN is optional for point-of-service or online transactions. Creating a PIN can be done in your online account through Settings, Debit Cards.
Yes, you can add your Benefits Card to Apple Pay®, Google PayTM or Samsung Pay® in a mobile wallet if your device offers that function.
If using at point of service, try running the purchase as a credit transaction and/or swiping or inserting your card in the terminal. If you’ve created a PIN, you can run the transaction as debit. Before using your card, always be sure to check your balance to ensure funds are available and that you’re paying for a qualified service or item. You can also pay for the expense(s) with your own funds, then submit a claim for reimbursement.
To easily and reliably check your balance anytime, log in to your online account or use the HSA Bank app.
The HSA Bank stacked card allows members to pay for healthcare-related expenses from several accounts using one debit card. Availability of the card has been proven to increase participation in benefit programs such as HSAs, FSAs and HRAs. In fact, 62% of cardholders reported that the availability of a card tied to these accounts influenced their decision to sign up. Because employee funds are contributed pre-tax, there’s savings to employers in FICA contributions. Associates also view this employee benefit favorably. Additionally, the employer's name can be included under the participant's name (within guidelines).
